 Dr. Yared Tekabe runs studies in cardiovascular disease detection and prevention at Columbia University. (Photo by Kidane Mariam for Tadias Magazine)
Dr. Yared Tekabe runs studies in cardiovascular disease detection and prevention at Columbia University. (Photo by Kidane Mariam for Tadias Magazine)
Tadias Magazine
By Tseday Alehegn
Published: Tuesday, March 17, 2009.
New York (TADIAS) – Dr. Yared Tekabe enjoys doing most of his reflections while sitting anonymously with his laptop at cafés in Harlem. When he’s not there, Tekabe is busy running studies in cardiovascular disease detection and prevention at his lab in Columbia University’s William Black building in upper Manhattan. Last November, Tekabe’s groundbreaking work on non-invasive atherosclerosis detection and molecular imaging was published in the American Heart Association’s journal, Circulation, along with an editorial citing its clinical implications.
Dr Tekabe’s success has helped his laboratory, headed by Dr Lynne Johnson, to receive another $1.6 million four-year grant from the National Institute of Health to continue his research, and Tekabe hopes that in a few years time his work can help heart disease prevention efforts and early detection of atherosclerosis in humans.
“What is atherosclerosis in layman terms?” I ask him, trying hard to correctly pronounce this tongue twister. He breaks it down to its linguistic roots. “Atherosclerosis comes from the Greek roots athere which means gruel, and skleros which means hardness or hardening,” he explains. Further research in Wiki reveals that atherosclerosis is a condition affecting our arterial blood vessels, which transport blood from the heart to the rest of the body. Atherosclerosis is the chronic condition in which inflammation of the walls of our blood vessels lead to hardening of the arteries.
“Atherosclerosis is the underlying cause of cardiovascular disease (CVD),” Tekabe says. “The result is progressive closing of the blood vessels by fat and plaque deposits, which block and further restrict blood flow. In more serious cases it may also lead to clots in the aorta (main artery coming out of the heart) or carotids (arteries supplying blood to the brain) that may dislodge and travel to other parts of the body such as the brain, causing stroke. If the clot is in the leg, for example, it can lead to gangrene. Deposits of fat and inflammatory cells that build up in the walls of the coronary arteries (supplying blood to the heart muscle) can rupture leading to blood clots. Such clots in an artery that supplies blood to the heart muscle will suddenly close the artery and deprive the heart muscle of oxygen causing a heart attack. In the case of very sudden closure of an artery a clot can cause sudden cardiac death.”
“It’s the Tim Russert story,” Tekabe says, providing a recent example of what undetected levels of plaque formation in our bodies can lead to. EverydayHealth.com, an online consumer health portal, had described the famed former MSNBC ‘Meet the Press’ host’s sudden heart attack as being caused by a plaque rupture in a coronary artery. Russert had previously been diagnosed with heart disease, but his atherosclerosis was asymptomatic. He had not experienced the common signs of chest pain and other heart attack symptoms to warn him or his doctors of his true condition. The undetected inflammation in his vessels and the subsequent rupture of plaque led to his sudden heart attack and untimely death. This is not uncommon, however. According to the Centers for Disease Control and Prevention (CDC), heart disease “is the leading cause of death for both women and men in the United States, and women account for 51% of the total heart disease deaths.” There is even more grim news: United States data for 2004 has revealed that the first physical symptom of heart disease was heart attack and sudden death for about 65% of men and 47% of women with CVD.
The risk factors for atherosclerosis are well known and Tekabe runs through the list with me: “diabetes, obesity, stress, smoking, high blood pressure, family history of CVD, and diet” he says. “But of all the factors that I have mentioned, I would say diet is the most important one to change,” he adds. Food items such as red meat, butter, whole milk, cheese, ice cream, egg yolk, and those containing trans fat all put us at higher risk for plaque formation. The American Heart Association recommends eating fish such as salmon, herring and trout instead of red meat, as well as eating food that is steamed, boiled or baked instead of fried. It is better to use corn, canola, or olive oil instead of butter, and to eat more fiber (fruit, vegetables, and whole grain). Notwithstanding that March is deemed National Nutrition Month by the American Heart Association, changing our diet is largely emphasized in CVD prevention. We should also be exercising at least 30 minutes each day.
“Early non-invasive detection of the presence of inflammation and plaque could save lives,” Tekabe points out. “But the problem is two-fold: those who suffer from atherosclerosis do not display warning signs until it’s too late, and for doctors, a non-invasive method of detecting atherosclerosis is by and large not a possibility.” Research by Tekabe and others may soon change the way doctors can detect atherosclerosis.
Using molecular imaging techniques that were previously popular in cancer biology research, Tekabe and his colleagues have discovered non-invasive methods of detecting RAGE, a receptor first discovered in 1992 and thought to have causative implications in a host of chronic diseases ranging from diabetes to arthritis. Tekabe, collaborating with Dr Ann Marie Schmidt who has shown that RAGE receptors play a key role in atherosclerotic inflammatory response, notes that these receptors can be detected non-invasively in mice that have been fed a high-fat, high cholesterol diet.
“In the past, although we knew about the RAGE receptor, especially in the study of diabetes, we were not able to detect it without performing an autopsy of the lab mice. Clearly, in the case of humans it would be pointless if we said that we detected atherosclerosis in the patient after the patient had died,” Tekabe explains. “Therefore, it was imperative that our research showed a more non-invasive method, detecting RAGE receptors and locations of inflammation while the subject was still alive. The first step would be to test it on mice, which we have, and then perhaps on larger animals such as pigs, so that this research could be successfully translated to help non-invasively detect atherosclerosis in its early stages in human beings.”
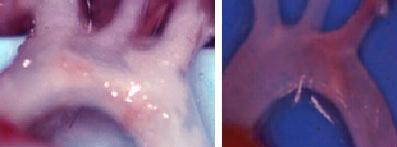
Left Image: Atherosclerotic aorta: The image is from a mouse fed a Western type of fat diet (high-fat, high cholesterol diet) for 34 weeks. It shows complete blockage of the aorta and the branches that supply the brain. The plaque is made up of fat and inflammatory cells.
Right Image: Relatively normal aorta: This is from 6 weeks old mouse fed a normal diet.
Tekabe’s recently published research showing detection of RAGE receptors responsible for arterial inflammation was funded by a grant from the American Society of Nuclear Cardiology as well as from an American Heart Association Heritage Foundation award.
The November Circulation editorial entitled “Feeling the RAGE in the Atherosclerotic Vessel Wall” highlights the significance of Tekabe et al’s findings and the necessity for early detection of atherosclerosis. “This is an exciting development that adds an important marker of atherosclerotic disease that can now be assessed non-invasively,” write Drs. Zahi Fayad and Esad Vucic. “Tekabe et al demonstrate, for the first time, the noninvasive specific detection of RAGE in the vessel wall.” They concur with Tekabe that “noninvasive detection of RAGE in the vessel wall could help define its role in plaque rupture, which has potentially important clinical implications.”
Tekabe came to Boston in 1990 and subsequently completed his Bachelor’s degree in Biotechnology and his Masters and PhD in Biomedical Sciences with a focus on CVD and drug development. His academic choices have inevitably led him to his career as a scientist, but he has personal reasons for choosing this path as well.
“I was born in Dire Dawa, Ethiopia. I have 1 brother and 8 sisters, and my parents had no formal education. But my father always encouraged me to seek higher education. While I was completing my studies I witnessed my beloved father suffer from Coronary Artery Disease (CAD) and he underwent triple bypass surgery. He passed away in 2004, and I promised myself that I would step up to the challenge of finding a way to prevent heart disease” Tekabe says in a somber and determined tone. “Heart disease is the leading cause of death in the developed world, and I am motivated by that challenge, but this research is also deeply personal.”
Tekabe hopes that his research will be applicable to other areas where RAGE receptors have been hypothesized to play a central role. Circulation editors who follow Tekabe’s work have noted that “in addition to its role in atherosclerosis and the development of vascular complications in diabetes, RAGE possesses wider implications in a variety of diseases, such as arthritis, cancer, liver disease, neurodegenerative disease, and sepsis, which underscores the importance of the ability of its noninvasive detection.” Tekabe, as part of Dr Ann Marie Schmidt’s team, has already filed U.S. and international patents and has plans to jump-start a drug development arm of the pharmaceutical industry in Ethiopia. “I’m looking for interested sponsors in Ethiopia who can see the potential of this research and its global implications,” he states.
Now that Forbes has apprised us of the billionaire status of an Ethiopian-born businessman, we hope this news may peak his interest in helping to start scientific research initiatives in Ethiopia.
—-
Join the conversation on Twitter and Facebook.


























Non-invasive atherosclerosis detection in humans would be a major break through in Medicine and would help prevent so many sudden deaths that occur as a result of heart attack, stroke and alike. Magnificent talents such as Tim Russert and a growing number of ordinary Ethiopian men and women, both here and especially in Addis, are dying young as result of the same medical problems. I really believe that in America and urban Ethiopia like Addis, we must change our diet to be healthy. Having said that, please allow me to congratulate you Dr. Yared on your groundbreaking research in Atherosclerosis! Keep up the good work. You are serving humanity via your education.
Dear Editor in Chief Tseday Alehegn: Also, please allow me to extend my best compliments for your wonderful penmanship and first class magazine. You are a talented young writer. I always follow your writing on Tadias. May god grace you with a very long life and your friends!
Great, uplifting personal story! Keep up the good work!!
This is really an exciting result. Congratulation on your work and publication. Finally i would like to send my great appreciation to Tseday for the wonderful presentation.
Tseday,
Very well explained in a simplified way. Great job!!!
It is ever so wonderful to see one of ours rise to the top as a research scientist. Whoever said that the Nobel Prize in medicine is a private reserve for the likes of Luc Montagniers of this world?
Sorry to hear the passing of your dad. Long,long before you were born a hometown poet wrote a few lines of verse about his friends and I think your beloved father was one of them. It went like this.
…………………
…………………..
GOBEZ AYDEL ESU SAK CHEWATA AYWEDE
YESERAL KELEBU TEKABE HABTEWELDE
…………………..
……………………..
Keep up the good work dear Yared! We are proud of you.
A source of inspiration and pride for other youg ethiopians both here and back in home.
Wishing the best of lucks for all Ethiopians struggling day and night for a better future. May God bless you.
Thank you so much, Tseday, for sharing this inspiring story and for allowing others to read and acknowledge the achievements of Dr. Yared Tekabe. Your article is so well written that it is educational. Thank you again for promoting and highlighting the accomplishment of this capable young man to your readers. It gives me a sense of pride when I read such kinds of encouraging stories about the achievements of my country people (!?) He is an inspiration and a role model for all and I hope your article will start our youth in the journey of the pursuit of excellence.
I am going to pass on the article.
Thank you Dr. Yared for this wonderful finding that will save people’s lives. God has shown you the light and you have followed it. I really honor your dedication. I am so proud of you. You are one of the Ethiopians who can make a big change in this World. This is the time.
Dear Tseday, I really loved your article. Keep on bringing more successful Ethiopian stories.
Great job!
Yes, we can!
&
Many Blessings.
Good job Dr.Yared
Dear Tseday Alehegn would you write about HIV awareness. I just want to mention about HIV and our community. I have a chance to spend five weeks in one of the HIV clinics in Metropolitan area of DC learning about HIV and the number of Ethiopians overwhelmed me. Even though the Ethiopian community is trying their best to spread the word, I don’t think our community is fully aware of the situation. Please Interview one of the Ethiopia Infectious Disease physicians in DC.
Thanks
Tazabe
Keep up the good work Doc. You are an inspirational to us all.
Dear Dr. Yared
I’ve read your publication on American Heart Association entitled “Feeling the RAGE in the Atherosclerotic Vessel Wall” published in November, 2008. I was very impressed and proud to see my brother’s hard work and dedication finally paid off.
Scientist like Dr.Yared is what Ethiopia needed at this point. Individual who has the source should work with young and intelligent people like him to restructure the the underlying framework of Ethiopian Medical facilities.
I honestly think that CAD is a common disease in Ethiopia. Finding a cure is the absolute solution. Please continue your hard work.
I congratulate you my brother, Dr. Yared for your hard work. Your dedication to Medicine is so vital to anyone in this planet. I am so honored to see my father’s dream fulfilled as well as yours.
Dear Editor in Chief Tseday Alehegn: You have done a wonderful job in documenting the article. I wish you all the success.
Hi dear Yared. I am wondwossen fiseha. I am proud because you are from my city and bgs school. I want to contact you also you can e-mail me wondwossen542@yahoo.com.
What a great story!!
Hi, Yared
I’m Martha Haile, Sister of Negede, Tegene and Mulatu Haile From Dire. I’ am so proud of you. I Can’t wait to let my family know about your great work and people who knows you since BGS or Notre Dame. If you can please contact me mhaile@clacorp.com.
Great job an inspirational story for all of us and our kids, we should all take note of our “Ethiopian diet” Kitfo and doro and the like. Try to live healthy
Congrats Dr. Yared! We are truly proud of the milestone you have reached so far. We are rooting for you to win a nobel prize. Ababeye is surely smiling from heaven. Keep up the great work. Tseday, as always, you are a brilliant writer, and I enjoyed your awesome journalistic style.
Congraaaaaaaaaaaaaaaaaaaats, Yaruca!
Dr. Rebka and your girls Liya and Helina Yared
Bravo Dr. Yared T. Great Work, Keep on Going and Going!!!
Many renowned researchers having spent all their lives discovering so many valuable fallouts for humankind on this planet. Yet, when they were on their last minutes to pass away they all invariably felt that they left so many unconquered research frontiers behind that they would have conquered for better livelihoods to humankind than their own. Yared, let us reassure you that you are now more conscientious than ever before to keep on working for more and more breakthroughs from you research work in the years to come.
Your Dad and we all believe that the Promised Land, the Heaven we all aspire to go to is here on this Earth. You have joined those researches who are working hard to bring healthy livelihoods to this planet in the future days to come and trust us that there will come days when we will all live happily without diseases, wars and hunger if work together.
We are proud about you and we wish you all the best.
Great work Tseday Alehegn, Tadias Magazine.
Amen Brother!!!
that is such a great, fantastic and intresting job Dr.Yared T.
i am really proud of you and your team.
so keep working on it, cause it is what we all need.
GOD BLESS YOU!!!
Congrats Dr. Yared. Your story about your dad was touching. He must be thrilled in heaven amongst all the prophets. We know even from science that energy never dies, but transforms itself from one form to another. He may not be with you physically, but he is with you spiritually.
DR.YARED CONGRADULATION
oh i can’t tell you how happy i am
I AM REALLY PROUD OF YOU
KEEP UP the GOOD WORK
MAY GOD BLESS YOU AND YOUR FAMILLY
Hello, Dr
I’m proud of you. keep up the good work.
How blessed to be a fabulous model for everyone.
Dr. Yared, may God help you to accomplish your influential goals.
Dear Dr. Yared, I congratulate you on your success in your paticular study. Well done!
Though I applaud the many wondeful things that medical science had given humanity, please, do allow me to share my concern regarding the ethical side of science in general.
I believe those, who do have the access to knowledge in conducting whatever research on/for humans should take the matter very seriously in terms of Ethic and moral.
Over the past three years, more than 60 institutions, including several of the
world’s most prestigious research centers, have been criticized by the U.S.
government for failing to protect human subjects adequately.
Conducting medical research on humans is a tricky business. It is not the same thing as providing risky but proven medical treatments, which is done for patients. Medical experimentation is done to test subjects in order to further science. The experimenters may hope to help the subjects, but since the procedures are, by definition, not fully tested, they also have potential to cause great suffering and harm. Obviously there are many medical experiments that lead to a dangerous moral trap that could result in society looking upon people with catastrophic conditions as usable commodities
Nowadays, large pharmaceutical companies distance themselves from the experiments on humans by outsourcing most of their trials to private test centers across the U.S. and around the world
Every year, we hear that several Ethiopian trial participants are injured or killed. The tragic part of the whole experimentation is that targeted individuals have no clue that they have been used as guinea pigs.
As Ethiopian Americans, I think everyone involved in higher medical or biological research, testing drugs on Ethiopians or using their blood and DNA for further experimentation, has a moral and spiritual obligation to inform the individual or the community – even if they have to lose their job or career aspirations.
I really admire those who work hard for the wellbeing of every human being!
omg…. i`m speachless! i was looking for some ethiopian art and i don`t know how i landed here but i`m realy glad i did good work.
hey..,i can`t say god bless you `coz, you already blessed.
Dr. Yared… you accomplish victory step by step… then the bright you are, the more blessing and success comes to you. I’m proud that my brother discovered the most wonderful job…. keep it up….we all Ethiopians loves you.
Dear Tseday,
You’re truly professional in presenting this complicated disease. You’re very talented.
Keep up the good work!!!
Brother Dr. Yared,
I congratulate you on your success. Your dedication and commitment to solving this disease is PRICELESS. I’m so proud of you. Your hard work will save so many lives in the world.
Tseday, your writing is flawless. I thank you so much for publishing Dr. Yared’s work.
Love Mimi.
Dear Dr. Yared
I am so proud of you… Usually anything that is posted about Ethiopia is the hunger, disease or War. I thank you so much for changing people’s view. Keep up the good work..
In response Abram’s note: I appreciate your response, but we need a positive vibe..
Regards
Solo
Congrats Yared,
I am very glad that people are recognizing your amazing work. I am going to be following your great accomplishments for years to come and I know that the best is yet to come. I hope that we will have many more coffees together at our beloved Harlem and can’t wait to hear your upcoming studies and aspirations.
Tseday, your writing is flawless. I read this article more than 5 times. Keep it up sister. I really admire those who work hard for the well being of every human being!
Dr Yared, you accomplish victory step by step I’m proud of you. keep up the good work.
Kid
Kidanefilms
Livity production,LLC
Oh BTW, It takes a talent and a touch of a prolific writer like Tseday to take a complex subject like this one and deliver it to us in such a layman’s term. My hat off to your writer and keep up the great work. I have bookmarked your site and become a frequent visitor.
Daniel
Hi Uncle Yared,
We’re very happy for your success. These is from all your families in Ethiopia.
Brgds Eyoel Girma, Rediet Girma, Nathnael Girma
This article was probably one of the most easily accessible pieces on medical research I have ever come across. The research that Dr. Tekabe is doing in the field of atherosclerosis detection seems essential in the fight against cardiovascular diseases and his research in relation to RAGE could lead to further discovery across the board of health issues that plague man today. As a senior in high school in the process of deciding on colleges and possible majors, I really appreciated this article’s insight on the life and work of one ethiopian professional. It was written for any layman to be able to understand and appreciate the research being described.
Congrats! keep up the good work.
Dear Dr. Yared Tekabe. I am proud to see one of my own family member rise up to be a great scientist. You are an inspiration and role model to our youth. In your spare time, which you may not have, could you speak to the youth? They need your uplifting story. Great job. Thank you for sharing.
This is a highly informative and ideally a life altering jar. Particularly for those of us who like to partake of the “Fatty” foods. This work is a rather graphic reminder for all of those who are still resistant to being health conscious in what they consume on a daily basis.I look forward to reading more ground breaking work from you in the future.
Much Kudo’s for this important contribution.
Dr Tekabe congratulations on your achievement in the field of medical research. One can achieve his or her goal if he or she puts heart and mind to it. And You did. I am proud of you. your work benefits all human kind and opens doors for your fellow young Ethiopians.
Dr Yared Tekabe. Congrats! I am really impressed with your remarkable medical research. Keep up the good work.
-Koni
Dr. Yared Tekabe
Good job. Everybody is proud of you. God bless you.
It is a wonderful work you did. I wish you more success in your life.
It is always a pleasure to see Ethiopians making major contribution in the scientific world. Dr. Yared’s remarkable research is a lesson to our reptilian brain that often craves unhealthy food. When I was done reading, I have already made a commitment to stay away from fast foods and “Gored Gored.”
I congratulate you on your impressive research and discovery. Identifying atherioscrelotic plaque non-invasively could save millions of lives by enabling medical professionals to detect potentially lethal illnesses early. It’s about time that we change our dietary culture and tame the urge or craving to consume immoderate amounts of foods high on bad cholesterol. But more important is to be able to educate and enlighten fellow Ethiopians back home. Wouldn’t it be wonderful if businesses like Sheraton Addis sponsored a symposium to be led by Dr. Tekabe aimed at imparting and sharing informaton with aspiring nutritionists, health profession trainees,etc. and involving media outlets (Eth. Tv, radio stations, newspapers)? What do you think? Let’s keep the idea alive! Tseday/Tadias: Thank you for the beautiful and effective presentation.
Thanks Tseday Alehegn, the article is well-written and uplifting story.
Yared, great job putting your talents to a worthy cause…
Thanks,
Teddy
Dear Dr.Yared, I congratulate you on your achievement in the field of medical research. You are an inspirational to many Africans, specially Ethiopian. I am so proud of you my dear friend. Keep up the good work my dear. God bless you and your family.
Congrats Yared! This is an inspiration for all of us. I dont think I can fully understand the depth of your as I am not in the field.
I feel so greatful for you Dr Yared, for this great research, to accomplish his goal on finding ways to diagnose early heart problems. Congratulation Dr and Job well done!!!!
Congratulations Dr. Yared, I am Proud of you. Keep up the good work
I always new there was something special about you. I feel so blessed knowing that my brother in law is about to become a famous scientist and multi millionaire. A party in Vegas for your achievements is way overdue.
Andy
I don”t know what to say but this issue as it touches all human beings so I am proud of you doctor Yared. You did a good job and god bless you. Cheers.
Thank you all so much for your great response. “Betam Amesegnalew”
First of all, I would like to thank the author Tseday for a wonderful job to reach out to an Ethiopian doctor who is doing a wonderful thing for everybody in this particular and important field to find and to expose to the world his achievements and his success. Dr. Yared is a role model to all of us. Hopefully very soon he will be a Nobel Prize recipient for the invaluable research that he is doing. Last but not least, I’d like to congratulate you for your good work and for representing all of us well to give us a source of pride as well as those who came before you in the past. Keep up being a role model and we all are very proud and appreciative of your work.
FDNY
Great article by Tseday. Dr Yared, we are all proud of you and as you blaze new trails in the groundbreaking research that you are doing, you remain a role model for future scientists.
Inspiring Article! From my conversations with Dr. Yared, I know he is a rising star!
I would also like to compliment Tseday on her writing!
Lastly, I would like to respond to a post by Abram (Mar 21st, 2009 at 9:36 am) concerning Research Ethics.
As a research scientist myself, I am well aware of the ethical issues behind doing research on humans. But before any research gets to clinical trials, a series of extensive toxicity and proof of principle experiments are carried out. Unfortunately, things cannot be stopped after animal studies since what works in animals does not necessarily work in humans (If it did, we would have developed a vaccine against HIV and cancer a long time ago).
For the vast majority, when drugs reach clinical trials, they should not be deadly since preliminary research should show that it is not toxic before getting to that stage. So unless you are referring to people doing research that is not regulated, it is very uncommon.
MM
This is really great. I’ll be very careful with my diet from now on.
Saying that this is great work is certainly an understatement!
It is so empowering to find our African brothers not only digging their way out of the status quo, but to get to the point where they are making their own discoveries and most importantly not forgetting to bring the knowledge to the motherland.
I am impressed, inspired and thankful for the likes of Dr. Tekabe.
Good bless, I know you can continue to make great things happen.
thank you Dr.yared It is wonderful work.keep up
the good work god bless you and your family
Dr.yared
it is wonderful work.
god bless you and your family
I went to the school you went to, Bisrate Gabriel of Dire Dawa, Dr Yared, and just want to let you assure you of the great pride you’ve brought to your school and your schoolmates. God Bless
Dear Dr Yared.
I don’t know that much about you. However, I am so proud of the inspirational job you are doing. As I have understood, you are the man with VISION. God bless you. Beside this, I am so thankful for Tseday for letting me know about Dr Yared through the article
Demisse
Deme_ze20@yahoo.com
Dr Yared,
Congrats on your amazing work, it is so uplifting to see your commitment to developing medical and scientific breakthroughs. We’re so proud of you!
Yared,
This is a wonderful work! I am sure it is a result of hours and hours of hard work. Enjoy and best wishes for the future!
tiruneh
Congratulation Dr. Tekabe! I am very proud of you; besides, I admire your motivation for this kind of research. What you are doing is a big deal for our world, and it is an alteration for our Country’s name too. I just say keep on it & God bless you!
Hey Dr. Yared,
I just heard you had a baby son… congrats for both your research and you new addition to your lovely family, and two daughters.
Kaku
Dr. Yared,
I am quite impressed and elated about your scientific research and significant contribution for humanity to conquer Atherosclerosis, a number one killer disease as we know it. More than anything else Yared, I must recognize and congratulate you for your VERY hard work and sacrifice over many years. You are very focused, disciplined and know exactly what you want to accomplish in life. These are some of your rare qualities which I am always inspired by. Thank you so much for making us feel so proud inspired indeed!
May the good Lord bless you and your family!
Cousin, Merid
I am really happy for you. keep doing the good work Yared!
I am proud of you and congratulation my friend.
Tseday and Dr. Yared, my New York people!! great article, please push as much as you can to expand the topic to the Ethiopian masses.. this is a serious issue witch you guys have enlightened me and I’m sure many others as well.. keep up the great work…
peace
Dr. Tekabe… I recently met you at work and did not realize that I was at the presence of greatness. I am honored to have met you and I would like to take this opportunity to congratulate you on your research and the many more to come……I am sure we have not heard the last from you.
maaza
Keep up the good work Dr Yared, it’s important you keep searching for ways to prevent the illness from occuring and also warn the youth before it happens…it has been a great pleasure having conversation with you as well as reading your research.
Dr.Tekabes; Congratulations on all your success and great achievements throught out your professional career. I look forward on reading more of your publications in the future.
First thing first, I would like to commend you for tremendous job you’re doing. Second, I think its eye opening and instructive critique. Most of us know craving for those fatty food had unprecedented side effect, yet we tend to pay no heed to it until it’s too late. I think it’s very serious diseases, fortified with lethal weapon. Dr. Yared we thank for your perseverance and commitment on your research, and I’m sure your exceptional work change people’s life ceaselessly.
I commend you for your hard work. It is an uplifting story. You have set an example and hope many more young Ethiopians follow your path.It is great accomplishment and keep up the good job.Thanks Tadias for sharing such great news and work with all of us.
Hey Yared,
I am so impressed and proud of your discovery! This is such great news, and coming from my uncle! I hope that this break through will help those in need and fulfill your dreams. I’m so happy for you Yared, and getting the chance to read about your work. I wish the best of luck to you! You make us all proud!!!
Mahlet Mesfin
Hey Yared. We expected nothing less. Very proud of what you’re doing, bro.
Hey Dr. Yared. We are all very proud of what you are doing and I hope the almight lord will enhance your knowledge to keep doing your work. keep-up Brother.
Dear Dr. Yared,
what is striking about your discovery is that you are very young:Indeed the future
is in your hands. I plead with young Ethiopians–where ever they may be– to take Dr.
Yared as their Model. His achievement goes beyond personal fame and wealth to benefit
humanity. In my humble openion, passionate intervention to help fellow human beings
ought to be the defining justification for our existence on this Earth !
Congradualation, Dr. Yared! Indeed, it has been a previlage to have met you,allbeit
by sheer accident .
Dr.Yared
This is, indeed, a great step for not only science, but also for human race as a whole. This one genius contribution for humanity can resolve the challenge our race- human race- is facing to survive withing the ups and downs of nature. As a result of your, Dr Yared, and your colleagues admirable effort, work and considerable moments of monotonous researching, significant amounts of pathetic deaths are guaranteed to be curtailed. I admire your and your teams work, plus your personal struggles to improve the duality of medical world. It is not long,I strongly believe, before I see you, furthermore, on CNN or BBC with Nobel prize for your deserving accomplishment. No doubt you will keep the excellence up; therefore, thank you, already, for your wonderful contribution for humanity, and I will look forward for the application of your empirically successful technique.
Y
Jobs well done Dr. I’m so proud of you.
hi yared befor i know your work or read your work i maet
you personaly by accedant and took me home which i left long long
time ago what a greet feeling .you are great not only in your reserch
your sence of humour too.keep up your hevenly work
Dr. Yared
You are doing an important work. It has value for all of us. Thank you.
selam
Tedi
Dr yared Tekabe , you are an Ethiopian hero! I lost my father to stroke! , as you know cardio and high blood pressure are the number one silent killers in Ethiopia , I hope your research will bring some good news , I wish you all the best and don’t forget that your father’s prayer in heaven also will help you, believe me!
Thank you all so much. I’ll update you on my progress with the help of God!
Tsedey,
Thanks for geting this complex issue in a simple term and for having an inspiring
interview with Dr. Yared. It is very enouraging for those in medical field to purue
in their studies keeping Dr. Yared as role model. Keep up the good work!!
Dr.Yared,
I’m happy that you have achieved this level of groundbreaking research on Heart Disease. Keep up the good work!
-Haikel
Good work keep up
taxiologist
Dr. Yared,
A belated congrats on your accomplishments.
Glad to see those long and grueling hours of studying finally paying off…
your old study companion from NU by way of Garden Street
Dr. Yared,
It is only by chance I came across this. It has been a very long time since we have talked. Your level of acheivement gave me not only a great pleasure but also remineded me of your aspirations and devotion to your work even when you were younger in high school and university. So, this is only the begining, I am sure you will do more……
Your old freind Zaki Kamil
I am Very proud of you. Keep up the good work and make us proud again and again. I am even more proud to have been born in Dire Dawa, like you!
It takes a great deal of effort to come up with such a breakthrough and it is my honor to have known such a great scientist. No doubt that this will not be last one because more shall come from you. I am really glad to come across you in person and have known you. I wish you all the best in your upcoming projects.
Dear Editor-In-Chief,
Many thanks foe the brilliant Article. keep up with the good work.
Dear Dr. Yared, It is indeed great to read about your cutting-edge research in combating coronary heart disease. The fact that your approach is non-invasive makes it even more exciting.Great job!
You’ve also highlighted the importance of adopting healthy habits during the interview, which is pivotal, if we want to win the war against heart disease and in general against non-communicable diseases such as cancer, diabetes etc.
I’ve developed a DVD in Amharic recently. “Teninet Bemircha” is a 75 minutes DVD with special emphasis on prevention of heart disease, cancer and diabetes. Prevention is indeed better than cure!
I specialize in lifestyle and preventive medicine and I would love to send you (and Ms. Tseday as well) a copy of it, if I could get your address.
It would be great to stay in touch with you
Be blessed
Dr. Dawit
It is a privillage to read about a fellow Ethiopian conducting groundbreaking research. It is truely a motivation and great pride. Thank you and keep up the good work Doctor.
You have done so much for the world. Thank you and keep up the good work.
We r so proud of u,’This time for Africa….!’
God bless u!
Menbere Tesfaye
We Ethiopianare proud of u Especially From DD
Great job
Hi, Dr.Yared , it is a great deal of work ,so proud of you .
great job . hop you will do more .